CPT codes are standardized codes used for medical billing and insurance purposes. They ensure accurate reporting of procedures like transrectal ultrasound-guided prostate biopsy. Recent updates include Category III codes for emerging technologies‚ reflecting evolving medical practices.
1.1 What Are CPT Codes?
CPT (Current Procedural Terminology) codes are standardized codes used to describe medical‚ surgical‚ and diagnostic services. They are essential for billing and insurance claims‚ ensuring accurate reporting of procedures like transrectal ultrasound-guided prostate biopsy. Developed by the AMA‚ these codes are regularly updated to reflect advancements in medical practices. Recent updates include Category III codes for emerging technologies‚ such as new biopsy techniques. CPT codes facilitate uniform communication among healthcare providers‚ payers‚ and patients‚ ensuring transparency and consistency in medical billing processes.
1.2 Importance of CPT Codes in Medical Billing
CPT codes are crucial for accurate medical billing and reimbursement. They standardize the reporting of procedures‚ ensuring clarity and consistency in claims submission. For transrectal ultrasound-guided prostate biopsy‚ CPT codes help providers bill correctly‚ reducing errors and delays. They also facilitate data analysis for healthcare policy and research. Updates to CPT codes‚ such as Category III codes for emerging technologies‚ ensure billing practices align with medical advancements. This system is vital for maintaining transparency and efficiency in healthcare billing and reimbursement processes.
Overview of Transrectal Ultrasound-Guided Prostate Biopsy
Transrectal ultrasound-guided prostate biopsy is a standard procedure for diagnosing prostate cancer. It involves using ultrasound imaging to guide tissue sampling. Despite alternatives like MRI-guided biopsy‚ TRUS remains widely used for its accuracy and accessibility. Ongoing clinical trials compare transrectal and transperineal approaches‚ aiming to optimize patient outcomes and reduce complications.
2.1 Definition of the Procedure
Transrectal ultrasound-guided prostate biopsy is a diagnostic procedure using ultrasound imaging to guide the collection of prostate tissue samples. It involves inserting an ultrasound probe through the rectum to visualize the prostate gland. A biopsy needle is then directed under real-time imaging to obtain tissue cores for histological examination. This method is widely used for diagnosing prostate cancer and assessing suspicious lesions. While it remains the standard‚ alternatives like MRI-guided biopsy are being explored to potentially reduce complications and improve accuracy in certain patient groups.
2.2 Purpose of the Biopsy
The primary purpose of a transrectal ultrasound-guided prostate biopsy is to diagnose prostate cancer by obtaining tissue samples for histological examination. It is used to assess suspicious lesions detected through elevated PSA levels or abnormal digital rectal exams. The procedure helps confirm malignancy‚ guide treatment planning‚ and rule out cancer in patients with ambiguous symptoms. While it remains the standard diagnostic tool‚ emerging alternatives like MRI-guided biopsy are being explored to potentially enhance accuracy and reduce complications in specific clinical scenarios.
2.3 How the Procedure is Performed
A transrectal ultrasound-guided prostate biopsy involves inserting an ultrasound probe into the rectum to visualize the prostate gland. Local anesthesia is typically administered to minimize discomfort. Guided by real-time ultrasound images‚ a biopsy needle is inserted through the probe or adjacent to it‚ allowing precise tissue sampling from suspicious areas; Multiple samples are collected for pathological examination. The procedure is minimally invasive and usually completed within 30 minutes‚ with patients often resuming normal activities shortly after. Proper sterilization and technique are crucial to reduce infection risks and ensure accurate diagnostic results.
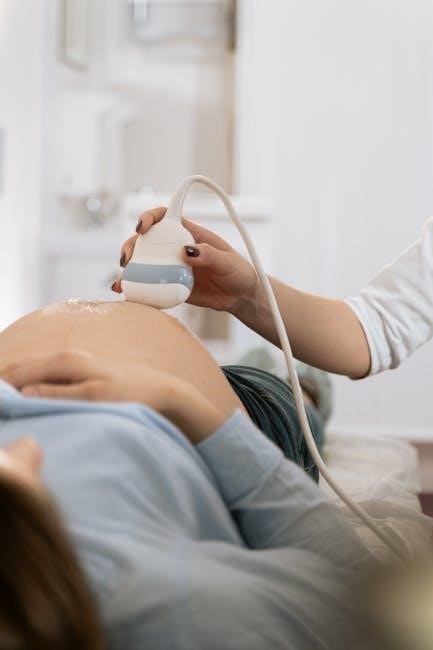
CPT Codes for Transrectal Ultrasound-Guided Prostate Biopsy
The primary CPT code for this procedure is 76942‚ representing ultrasound guidance for prostate biopsy. The AMA has approved Category III codes for emerging technologies in this field.
3.1 Primary CPT Code for the Procedure
The primary CPT code for transrectal ultrasound-guided prostate biopsy is 76942‚ which includes ultrasound guidance for needle placement. This code is essential for billing purposes and ensures accurate reimbursement. It specifically covers the imaging component of the procedure‚ distinguishing it from surgical codes. Category III codes are also relevant for emerging technologies in this field‚ as approved by the AMA. Proper use of these codes ensures compliance with billing standards and reflects advancements in prostate biopsy techniques.
3.2 Additional Codes for Related Services
Beyond the primary CPT code‚ additional codes may be required for related services. For example‚ CPT 77002 is used for MRI guidance if employed alongside ultrasound. Codes like 55700 may apply for biopsy procedures‚ while E/M codes (e.g.‚ 99213-99215) are used for patient consultations. Category III codes are also relevant for emerging technologies‚ such as advanced imaging or robotic-assisted techniques. Proper documentation ensures accurate billing for all services provided during the procedure‚ aligning with AMA guidelines and payer requirements. These codes complement the primary procedure code‚ ensuring comprehensive reimbursement.
3.3 Coding Guidelines and Specifics
Accurate coding for TRUS-guided prostate biopsy requires adherence to specific guidelines. The primary CPT code must reflect the procedure’s complexity and imaging guidance. Additional codes for imaging‚ complications‚ or concurrent services should be appended when applicable. Modifiers may be necessary to indicate bilateral procedures or repeat services. Documentation must include the number of biopsy samples‚ imaging modalities used‚ and any complications encountered. Coding should align with AMA and CMS updates‚ ensuring compliance with payer policies. Proper sequencing of codes and detailed reporting are essential to avoid denials and ensure accurate reimbursement. Stay updated on coding revisions to maintain compliance.

When to Use the CPT Code for TRUS-Guided Biopsy
Use the CPT code for TRUS-guided biopsy when diagnosing prostate cancer‚ especially for targeted biopsies. It is standard when MRI is unavailable or for specific clinical scenarios.
4.1 Indications for the Procedure
TRUS-guided prostate biopsy is indicated for diagnosing prostate cancer in men with elevated PSA levels or abnormal imaging. It is used for targeted biopsies of suspicious lesions and for assessing prostate cancer staging. The procedure is also employed in active surveillance protocols to monitor prostate health. Recent studies highlight its role in cases where MRI-guided biopsy is not feasible‚ ensuring accurate tissue sampling for histological diagnosis. It remains the standard approach for obtaining prostate tissue‚ especially in clinical scenarios where other methods are unavailable or less effective.
4.2 Clinical Scenarios Where the Code Applies
TRUS-guided prostate biopsy is commonly used for men with elevated PSA levels‚ suspicious imaging findings‚ or abnormal digital rectal exams. It is also applied in cases of prostate cancer staging‚ active surveillance protocols‚ and targeted biopsies of specific lesions. Recent studies highlight its use in scenarios where MRI-guided biopsy is not feasible or available. The procedure is particularly relevant for initial diagnosis‚ monitoring of prostate health‚ and in clinical trials comparing biopsy techniques. It remains a standard approach in urology for obtaining tissue samples when other methods are contraindicated or less effective.
4.3 Exclusions and Exceptions
The CPT code for TRUS-guided prostate biopsy does not apply to transperineal approaches or MRI-guided procedures. It excludes cases where biopsy is performed solely for research purposes‚ such as in clinical trials like the OPTIMUM study. Additionally‚ it does not cover complications or additional imaging services unless specifically coded; Exceptions include scenarios where ultrasound guidance is not used or when alternative techniques like MRI are employed. Coding varies if the procedure is part of comparative studies or emerging technologies‚ requiring Category III codes for new methods under evaluation.
Billing and Documentation Requirements
Accurate documentation is essential for correct coding‚ ensuring compliance with AMA guidelines and payer requirements. Detailed records of the procedure‚ including imaging and biopsy details‚ are necessary.
5.1 Necessary Documentation for Accurate Coding
Accurate documentation is critical for correct coding of transrectal ultrasound-guided prostate biopsy. Key elements include patient history‚ procedure details‚ and imaging reports. Documentation must confirm the use of ultrasound guidance and biopsy sampling. Compliance with AMA and CMS guidelines ensures proper reimbursement. Records should also note any complications or additional services provided. Emerging techniques‚ such as MRI-guided biopsies‚ may require supplementary documentation. Clinicians must maintain detailed records to support coding accuracy and adhere to payer-specific requirements‚ ensuring seamless billing and reimbursement processes.
5.2 Billing Process and Payer Requirements
The billing process for transrectal ultrasound-guided prostate biopsy requires submission of the primary CPT code (76942) along with supporting documentation. Payers may require additional codes for imaging guidance or biopsy samples. Medicare and private insurers have specific requirements for reimbursement‚ including documentation of medical necessity. Providers must verify payer-specific guidelines to ensure accurate billing. Emerging technologies‚ such as MRI-guided biopsies‚ may require additional coding. Compliance with payer rules is essential to avoid claim denials and ensure timely reimbursement for the procedure.
5.3 Common Errors to Avoid
Common errors in billing for transrectal ultrasound-guided prostate biopsy include using incorrect CPT codes for imaging guidance or biopsy samples. Missing documentation of medical necessity can lead to claim denials. Another error is failing to append modifier codes when required. Incorrect reporting of multiple procedures or services can also result in payment issues. Additionally‚ not staying updated on coding changes‚ such as new Category III codes for emerging technologies‚ can lead to compliance violations. Ensuring accurate and complete documentation is crucial to avoid these pitfalls and ensure proper reimbursement.
Reimbursement and Payment Rates
Reimbursement for transrectal ultrasound-guided prostate biopsy varies by payer‚ with Medicare and private insurers having specific rates. Accurate coding and documentation are critical for timely payment.
6.1 Medicare Reimbursement for the Procedure
Medicare reimbursement for transrectal ultrasound-guided prostate biopsy is determined by the Physician Fee Schedule‚ which assigns relative value units (RVUs) to specific CPT codes. The primary code for this procedure‚ 76942‚ includes ultrasound guidance and imaging services. Reimbursement rates vary by geographic location due to regional cost adjustments. Accurate coding and documentation are essential to ensure proper payment. Additionally‚ Medicare may cover related services when medically necessary‚ such as laboratory analysis of biopsy samples.
6.2 Private Payer Reimbursement Rates
Private payer reimbursement rates for transrectal ultrasound-guided prostate biopsy vary depending on the insurer and negotiated contracts. The primary CPT code‚ 76942‚ is generally covered‚ but payment amounts differ. Factors influencing reimbursement include the payer’s fee schedule‚ geographic location‚ and facility or physician charges. Some private payers may also cover additional services‚ such as imaging or laboratory tests‚ when billed appropriately. Accurate documentation and coding are essential to avoid claim denials. Reimbursement rates are typically higher in outpatient settings compared to hospital-based care‚ though this can vary by payer policies.
6.3 Factors Influencing Reimbursement
Reimbursement for transrectal ultrasound-guided prostate biopsy is influenced by several factors‚ including payer policies‚ geographic location‚ and facility type. Clinical trial outcomes‚ such as those from the OPTIMUM trial‚ may impact coverage decisions. Emerging technologies‚ like MRI-guided biopsy‚ could alter reimbursement trends. Additionally‚ updates to CPT codes‚ such as new Category III codes‚ may affect payment rates. Accurate documentation and adherence to coding guidelines are critical to ensure proper reimbursement. Payer-specific negotiated rates and patient demographics also play a role in determining final reimbursement amounts for this procedure.

Comparison with Other Prostate Biopsy Techniques
Transrectal ultrasound-guided biopsy is compared to transperineal and MRI-guided methods. Each technique has distinct advantages‚ with transperineal reducing infection risks and MRI offering improved accuracy in targeting lesions.
7.1 Transperineal vs. Transrectal Approach
The transperineal approach reduces infection risks compared to transrectal‚ offering improved accuracy and faster recovery. However‚ it is more invasive‚ requiring anesthesia. Ongoing trials‚ like the OPTIMUM study‚ compare micro-ultrasound and MRI-guided biopsies‚ potentially shifting standards. Researchers highlight these differences‚ aiming to optimize patient outcomes and minimize complications. The transperineal method is gaining traction due to lower infection rates‚ while transrectal remains widely used for its accessibility. Both techniques aim to enhance diagnostic precision‚ but their clinical applications vary based on patient needs and institutional preferences.

7.2 MRI-Guided vs. Ultrasound-Guided Biopsy

MRI-guided biopsy offers superior visualization of prostate lesions compared to ultrasound-guided methods‚ reducing false negatives and targeting suspicious areas more precisely. However‚ it is more complex and costly. Ultrasound-guided biopsies‚ like TRUS‚ remain the standard due to their accessibility and lower resource requirements. Recent studies‚ such as the OPTIMUM trial‚ compare MRI and micro-ultrasound techniques‚ highlighting potential advancements in diagnostic accuracy. While MRI shows promise‚ ultrasound-guided methods are still widely preferred for their practicality and established efficacy in prostate cancer detection.

7.3 Coding Differences Between Techniques
Transrectal ultrasound-guided biopsy uses specific CPT codes‚ such as 76942‚ for image-guided biopsy procedures. MRI-guided biopsies‚ in contrast‚ may involve codes like 77085 or 77086 for MRI guidance. The choice of code depends on the imaging modality and procedure specifics. Category III codes‚ such as those for emerging technologies‚ may apply to innovative techniques. Recent clinical trials‚ like the OPTIMUM study‚ highlight advancements in biopsy methods‚ potentially influencing future coding updates to reflect improved diagnostic accuracy and efficiency in prostate cancer detection.
Clinical Trials and Research Updates
Ongoing studies‚ like the OPTIMUM trial‚ compare micro-ultrasound with MRI for prostate biopsy accuracy. These trials aim to enhance diagnostic precision and may influence future coding updates for emerging technologies.
8.1 Ongoing Studies on Prostate Biopsy Techniques
Research‚ such as the OPTIMUM trial‚ evaluates micro-ultrasound and MRI for prostate biopsy accuracy. These studies aim to improve diagnostic precision and reduce complications. Additionally‚ clinical trials compare transperineal and transrectal approaches‚ focusing on infection rates and accuracy. The goal is to enhance patient outcomes and establish evidence-based standards for biopsy techniques‚ potentially influencing future coding updates and clinical guidelines.
8.2 Impact of New Technologies on Coding
New technologies‚ such as advanced imaging and laser-based systems‚ are influencing CPT coding. The AMA has approved Category III codes for emerging technologies‚ reflecting their growing role in prostate biopsy. Innovations like multiparametric MRI and micro-ultrasound are reshaping biopsy practices‚ requiring updated coding guidelines. These advancements ensure accurate billing for novel procedures‚ promoting transparency and consistency in medical billing. As technologies evolve‚ coders must stay informed to apply the correct codes‚ ensuring proper reimbursement and compliance with regulatory standards.
8.3 Recent Findings and Recommendations
Recent studies‚ such as the OPTIMUM trial‚ highlight advancements in prostate biopsy techniques. Data presented at the European Association of Urology Congress suggest improved accuracy with micro-ultrasound and MRI-guided methods. Researchers recommend adopting these technologies to reduce complications and enhance diagnostic precision. Updated coding guidelines are essential to reflect these advancements‚ ensuring accurate billing and reimbursement. Clinicians are encouraged to stay informed about emerging techniques and their coding implications to maintain compliance and optimize patient outcomes in prostate cancer diagnosis.
Coding for Complications and Related Procedures
Coding for complications‚ such as infections or bleeding‚ requires specific CPT codes. Additional imaging services and follow-up care must be accurately documented for proper billing and reimbursement.
9.1 Coding for Infections or Bleeding
Infections or bleeding post-procedure require specific CPT codes. Use E&M codes for evaluations and management of complications. ICD-10 codes are needed for conditions like prostatitis or hemorrhage. Accurate documentation linking the complication to the biopsy is essential for proper reimbursement. Additional codes may apply for antibiotic therapy or blood transfusions. Ensure compliance with payer guidelines for reporting these complications. Proper coding prevents claim denials and ensures timely payment for related services.
9.2 Coding for Additional Imaging Services
Additional imaging services‚ such as MRI or ultrasound‚ require separate CPT codes. For MRI-guided procedures‚ use 74185 for abdominal MRI or 77058 for MRI guidance. Ultrasound imaging beyond the primary biopsy may require 76942 for ultrasound guidance. Ensure documentation supports the medical necessity of these services. Payer guidelines may vary‚ so verify requirements before billing. Accurate coding ensures proper reimbursement for imaging services provided alongside the biopsy. Always link imaging codes to the primary procedure for clarity and compliance with billing standards.
9.3 Coding for Follow-Up Care
Follow-up care after a transrectal ultrasound-guided prostate biopsy requires specific coding. Use E/M codes (e.g.‚ 99213 or 99214) for office visits. If complications arise‚ additional codes like 76942 for imaging or 77002 for fluoroscopic guidance may apply. Document patient monitoring and any interventions. Payer policies vary‚ so verify requirements. Accurate coding ensures proper reimbursement for post-procedure care. Link follow-up services to the primary biopsy for clarity. Stay updated on coding guidelines to reflect current practices and technologies‚ such as emerging trends in biopsy techniques discussed in clinical trials like the OPTIMUM study.

Future of Prostate Biopsy Coding
Emerging technologies and clinical trials‚ like the OPTIMUM study‚ are reshaping prostate biopsy coding. AI and robotics may introduce new codes‚ enhancing precision and efficiency in billing.
10.1 Emerging Trends in Prostate Biopsy Techniques
Emerging trends in prostate biopsy techniques include the use of micro-ultrasound and MRI-guided biopsies‚ as highlighted in the OPTIMUM trial. These methods aim to improve accuracy and reduce complications. Transperineal biopsies are gaining traction due to lower infection risks. Additionally‚ advancements in AI-driven imaging and robotic-assisted systems are transforming the field. These innovations may lead to new CPT codes‚ reflecting the evolution of diagnostic practices. Researchers and clinicians are closely monitoring these developments to optimize patient outcomes and streamline billing processes.
10.2 Potential Updates to CPT Codes
Potential updates to CPT codes for prostate biopsy techniques are expected due to advancements in diagnostic methods. The AMA has approved Category III codes for emerging technologies‚ such as micro-ultrasound and MRI-guided biopsies. Clinical trials‚ like the OPTIMUM study‚ may influence future code revisions. As transperineal biopsies gain acceptance‚ new codes could be introduced to differentiate this approach. Additionally‚ the integration of AI and robotics may require updated coding to reflect these innovations. These changes aim to align billing practices with modern medical advancements‚ ensuring accurate reimbursement for evolving techniques.
10.3 Impact of AI and Robotics on Coding
The integration of AI and robotics in prostate biopsy procedures is revolutionizing coding practices. These technologies enhance precision and efficiency‚ potentially requiring new CPT codes to reflect their use. As AI-driven systems become more prevalent‚ coding guidelines may expand to include specific identifiers for robotic-assisted biopsies. This evolution ensures accurate billing and reimbursement for advanced techniques. Staying updated with AMA guidelines will be crucial for coders to adapt to these innovations and maintain compliance with evolving standards in medical billing.
Resources for Further Information
Visit the American Medical Association (AMA) website for updates on CPT codes. Clinical trials‚ such as the OPTIMUM trial‚ and professional urology forums provide additional insights.
11.1 AMA Guidelines and Updates
The American Medical Association (AMA) provides detailed guidelines for CPT coding‚ including updates for transrectal ultrasound-guided prostate biopsy. The AMA recently approved a Category III code for emerging technologies in prostate biopsy‚ reflecting advancements in diagnostic procedures. These updates ensure accurate billing and reflect current medical practices; The AMA also offers resources on coding for transrectal ultrasound-guided biopsy‚ emphasizing proper documentation and adherence to guidelines. Regular updates are available on the AMA website‚ ensuring coders stay informed about the latest changes in prostate biopsy coding.
11.2 CMS Resources for Billing and Coding
The Centers for Medicare & Medicaid Services (CMS) provides essential resources for accurate billing and coding of transrectal ultrasound-guided prostate biopsy. The CMS website offers detailed guidelines‚ including updates on CPT codes and Medicare coverage policies. The Medicare Claims Processing Manual outlines specific instructions for billing prostate biopsy procedures. CMS also releases regular updates and training materials to ensure compliance with coding standards. These resources help healthcare providers navigate complex billing requirements and ensure proper reimbursement for procedures like transrectal ultrasound-guided biopsy.
11.3 Professional Organizations and Forums
Professional organizations like the American Medical Association (AMA) and American Urological Association (AUA) provide valuable resources for coding and billing. These organizations offer updates on CPT codes‚ including those for transrectal ultrasound-guided prostate biopsy. Forums and conferences‚ such as the European Association of Urology Congress‚ share insights from clinical trials like the OPTIMUM study. These platforms help healthcare professionals stay informed about coding guidelines and emerging techniques‚ ensuring accurate billing and compliance with industry standards. They also facilitate discussions on best practices for procedures like TRUS-guided biopsy.
Accurate CPT coding for transrectal ultrasound-guided prostate biopsy ensures proper billing and patient care. Staying updated with AMA guidelines and clinical advancements is essential for compliance and efficiency.
12.1 Summary of Key Points

CPT codes are essential for accurate billing of transrectal ultrasound-guided prostate biopsy. The primary code for this procedure is 76942‚ with additional codes for related services. Proper documentation ensures compliance and reimbursement. Clinical trials‚ like the OPTIMUM trial‚ compare biopsy techniques‚ influencing future coding practices. Staying updated with AMA guidelines and emerging technologies is crucial for accurate coding. Understanding indications‚ exclusions‚ and coding guidelines ensures correct application of CPT codes‚ optimizing reimbursement and patient care.

12.2 Final Thoughts on Accurate Coding Practices
Accurate coding for transrectal ultrasound-guided prostate biopsy requires precise use of CPT codes like 76942 and adherence to guidelines. Staying informed about updates‚ such as Category III codes for emerging technologies‚ is vital. Clinical trials‚ like the OPTIMUM trial‚ highlight advancements in biopsy techniques‚ which may influence future coding practices. Proper documentation and understanding of payer requirements ensure seamless billing. Continuous education and adherence to AMA and CMS guidelines are essential for maintaining compliance and optimizing reimbursement in this evolving field.
